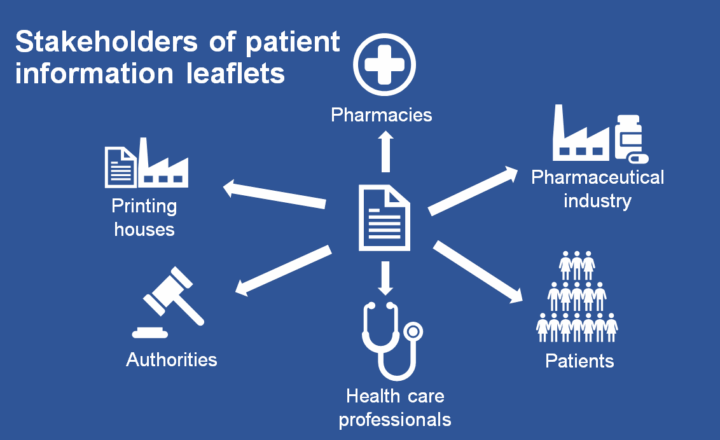
Stakeholders’ different requirements toward patient information leaflets
LifeFactFuture project’s work package 2 on manufacturing excellence includes a task that investigates ways to promote sustainability in life sciences manufacturing. One of life science manufacturing firms’ concerns deals with the consumption of paper in patient information leaflets that are included in medicine packages. Would there be a way to replace the paper leaflets with electronic solutions, and how, through which steps?
Researchers at University of Turku’s Industrial Engineering and Management unit conducted a literature review and organized workshops with LFF consortium partners to identify different stakeholders’ expectations toward patient information leaflets and possible steps in the transition toward electronic solutions.
Sustainability driving changes in supplying patient information
Traditional paper-based patient information leaflets included in medicine packaging represent a significant source of paper consumption and avoidable waste. Due to repeated purchases of the same medicines, patients know the basic features of their medication and do not read the leaflets at all, which implies that most of the leaflets are trashed immediately, without reading. This is an evident source of paper waste and causes an environmental sustainability challenge. In addition to environmental impacts, maintaining printed patient information leaflets requires considerable operational effort across the life sciences sector. Ensuring that every package contains an up‑to‑date leaflet involves continuous version control, production adjustments, and manual processes that introduce both cost and complexity.
The regulations concerning medication information, however, are quite strict and generally require that the patient information leaflet is readily available in the packages. At the same time, there are increasing pressures toward information accuracy, target group specific solutions, and frequent updates based on topical information. Electronic patient information leaflets have been suggested as solutions for these kinds of pressures, either through replacing the paper-based leaflet or complementing it. Ongoing research and pilot projects are examining various digital solutions, including the use of QR codes and integration with healthcare systems. Early experimentation within hospitals and healthcare professional workflows indicates that digital formats can effectively support clinical practice while significantly reducing paper use.
Different stakeholders’ requirements
End users, that is, patients are in a key position, when considering the replacement of paper-based patient information with an electronic solution. For some patients, the accessibility, timeliness, and possibility for personalization in the electronic solutions may be lucrative. Yet, there are large patient groups such as elderly people and those without access to digital tools who do not have an interest toward electronic solutions. Furthermore, the privacy requirement, requirement of information reliability, and infrastructural requirements in different countries may become obstacles for the electronic solutions.
Healthcare personnel and pharmacies in some countries are already experimenting with alternatives of paper-based information leaflets. The possibility for real-time updates and related improved medication safety are important for them. Reduction of waste and streamlining of workflows would be convenient. However, there are quite significant technical barriers that will require solving, both in pharmacies and hospitals. Who would carry the responsibility for the digital underlying solutions, and how would the systems interact in the global arena? Do personnel have sufficient capabilities and access to reliable digital infrastructures? Training, reliable access, and interface coordination with existing digital infrastructures are needed.
Including a patient information leaflet in medicine packages is one phase in the life sciences manufacturing process and a waste-producing task. Paper manufacturing, printing, and the packaging process consume energy, and this consumption could be reduced through using electronic solutions. However, adopting electronic solutions requires significant operational changes. Companies must redesign supply chains, update content management systems, ensure multilingual alignment, reorganize workflows, and retrain personnel to work with digital formats. Importantly, there will remain the concern for responsibility and reliability. Who is responsible, if something goes wrong in offering crucial medication information for patients?
Regulatory authorities form the backbone of this transition. In the EU and globally, they set the legal and structural requirements that ensure patient safety. Regulators currently emphasize a phased and inclusive approach to digitalization to avoid disadvantaging vulnerable populations. They aim to establish harmonized standards for electronic patient information leaflets, define rules for data protection, and ensure that manufacturers and health authorities remain the sole authorized editors of product information.
Roadmapping the path toward electronic patient information leaflets
LifeFactFuture project’s sustainability workshops revealed a shared desire to proceed toward offering electronic patient information leaflets at least in parallel to paper-based versions and experimenting with suitable target groups to identify opportunities for complete replacements. The immediate actions could focus on identifying pilot therapy groups and medicines for such experiments, assess patient needs, study user expectations and experiences, and prepare for the practical packaging changes. In order to build foundations for regulatory changes, there is a need to engage in lobbying toward the right stakeholders internationally and identify requirements toward the digital platforms that could be shared across countries, at least in Europe.
In a few years timespan, there is a need to engage in international networks to develop a Europe-wide platform for the possible electronic medication information solution. This requires agreeing on the rules and formats concerning the shared system, and likely also some incentive systems to motivate all stakeholders to participate. At the same time, pharmacies’ role in comprehensive care would need to be considered carefully, patient surveys and further experimentation would be needed, and training among all target groups. It is likely that the emergence of appropriate information systems and practical solutions will take years.
Throughout the patient information leaflet transition, environmental sustainability remains a major driver. Reducing paper waste, eliminating continuous reprinting cycles, and streamlining supply chains support broader climate goals and improve operational efficiency. However, technical resilience, such as ensuring backup access in areas with limited connectivity (archipelagos, ships, remote regions) must be built into system design. In parallel, trust, accountability, and transparency are essential, stakeholders must clarify who is responsible if digital information is unavailable, incorrect, or inaccessible. Overall, the workshops highlighted that a successful transition to ePILs requires a coordinated, multi‑stakeholder approach.
Harmonization of international guidelines and broad adoption among pharmacies, hospitals, and manufacturers will take time. Research and education are needed in many fronts, not just in the technical side but also concerning the human-related risks and patients’ willingness to accept digital solutions.
Miia Martinsuo
Professor, miia.martinsuo@utu.fi
University of Turku, Industrial Engineering and Management
Maarit Päällysaho
Doctoral Researcher, maarit.paallysaho@utu.fi
University of Turku, Industrial Engineering and Management